Key Takeaways:
~ Rosacea is an inflammatory skin condition that causes facial redness.
~ Increased inflammatory activation due to various environmental factors causes redness, increased vascularization and altered skin permeability.
~ Genetic variants associated with increased inflammation and vascularization are associated with rosacea.
~ Understanding your genetic susceptibility can help you find the right solution for your skin.
Members will see their genotype report below, plus additional solutions in the Lifehacks section. Consider joining today.
What is rosacea?
Rosacea is a chronic, inflammatory skin condition on the face that causes redness and irritation. It is three times more common on the cheeks and chin in women than men, while men are more likely to have the nose affected.
Everything you read about rosacea says something along the lines of “the exact causes of rosacea are not understood” and it is incurable…[ref] This doesn’t seem to be true, though, based on what is found in research studies.
Studies clearly outline the factors that cause rosacea. Activation of the immune system and vascular changes are at the heart of rosacea. Genetic variants play a role, of course, as does the skin microbiome. And research studies also show that there are a lot of ways to put rosacea into remission. Not every treatment or lifestyle change works for everyone, so it can take a bit of experimentation to figure out what works for you. The key takeaway here is that understanding your genetic variants and their role in inflammation and skin permeability may point you toward the right solutions for your skin.
Let’s take a look at the research on what causes rosacea, how it is defined, and the genetic variants that increase susceptibility.
Four subtypes of rosacea:
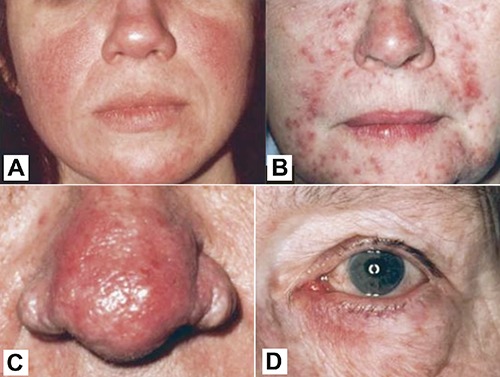
Rosacea is divided into four types, each with different characteristics:
- Erythematotelangiectatic rosacea: facial flushing, redness, visible capillaries
- Papulopustular rosacea: facial redness with inflammatory bumps that kind of look like acne
- Rhinophyma (phymatous rosacea): thickened, red skin on the nose that may be bumpy, waxy, and have visible blood vessels
- Ocular rosacea: watery, bloodshot eyes with redness on the eyelids.
Rosacea doesn’t always fit neatly into categories. Many people have multiple subtypes or fluctuate between types.[ref]
Burning, stinging, and overly sensitive skin also comes with rosacea, making it difficult to find skincare solutions that help rather than aggravate the condition. People with rosacea often have visible small blood vessels close to the skin. This is called telangiectasia – the small, dilated blood vessels that are usually visible on the nose and cheeks.
Red, bumpy nose in older men: Rhinophyma
Rhinophyma is the name given to a red, bumpy, thickened nose that is often seen in men over the age of 50. Many people think it is caused by drinking too much alcohol, but it is actually a type of rosacea.
I think this is a change that older men overlook because they don’t know what’s causing it — and they don’t know that there are readily available treatments for it.
Causes of rosacea:
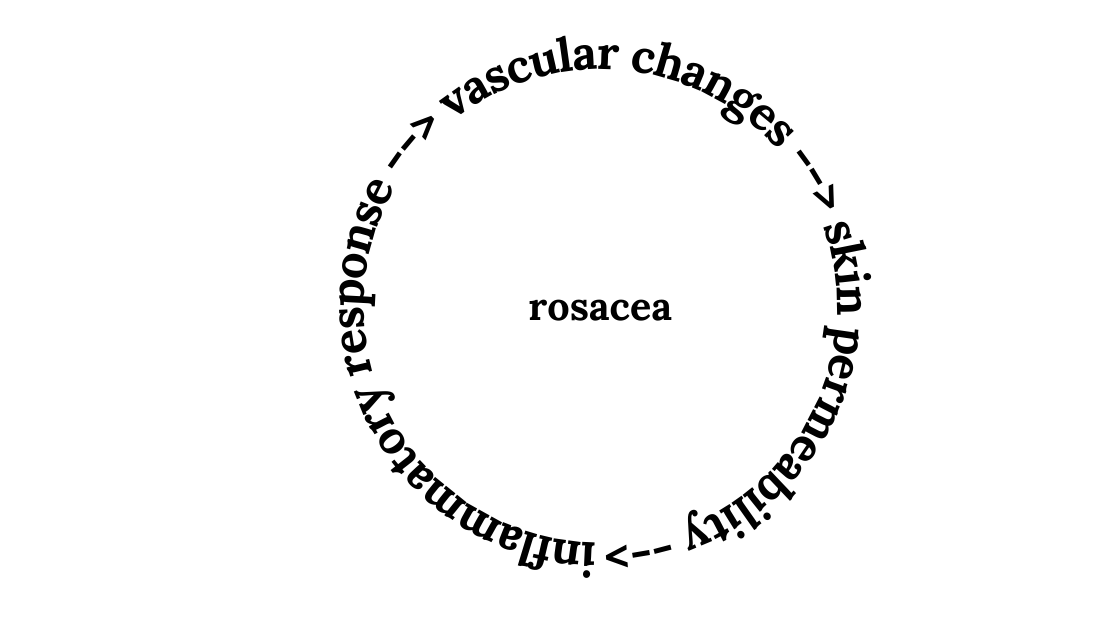
Research reveals that the cause of rosacea is a combination of overactivation of inflammatory pathways, changes in tiny blood vessels of the face, and changes in the tight junctions between skin cells.
Overactivation of inflammatory pathways includes the activation of toll-like receptors (TLR-2) and the activation of mast cells. The activation of mast cells releases histamine, which causes blood vessel dilation and permeability. Inflammation increases skin permeability, leading to more irritation from environmental factors and the skin microbiome, feeding into more inflammatory cytokine production.
Inflammation and immune system dysfunction:
In rosacea, there is an overactive response in the immune system that reacts to environmental and microbial factors on the skin. Many studies show that cathelicidin, an antimicrobial peptide, is overactive in rosacea, and it can trigger a cascade of inflammatory processes including mast cell activation. Kallikrein (KLK) 5 is the main serine protease that converts cathelicidin into LL37, the active version of cathelicidin that is abundant in rosacea skin. [ref]
Mast cells :
Mast cells are part of the immune system’s first line of defense against invaders. Activation of mast cells causes the release of histamine and other vasodilators and inflammatory cytokines, such as in allergic reactions. Mast cells are abundant in areas of the body exposed to foreign invaders, such as the skin, lungs, and intestines.
The MRGPRX2 receptor on mast cells is activated by cathelicidin, triggering inflammation and vasodilation. Animal studies show that when the MRGPRX2 receptor on mast cells is blocked, rosacea doesn’t develop.
Related article: MRGBRX2 receptor, genetics
TRPV channels:
Research shows that TRPV channels are also upregulated in rosacea. TRPV channels are ion channel receptors found throughout the body with a number of different functions, such as sensing pain or temperature. The TRPV4 ion channel has been specifically linked to rosacea and is upregulated in the skin where rosacea occurs. TRPV4 is activated by heat and also interacts with mast cells to send signals based on inflammation. Activation of TRPV can increase blood vessel formation as well as send the signal for the burning or irritated skin sensation.[ref]
TLR4, TLR2, and oxidative stress:
Toll-like receptor 4 is also elevated in rosacea, particularly in ocular rosacea. Oxidative stress (high ROS) is also implicated in causing ocular rosacea.[ref]
Toll-like receptor 2 is also found to be upregulated in the skin of rosacea patients. Activation of TLR2 leads to the production of cathelicidin (and LL37).[ref]
NLRP3 inflammasome activation:
Recent research suggests that the NLRP3 inflammasome pathway, which causes inflammation to be generally upregulated in tissues, is involved in rosacea. Importantly, NLRP3 inhibitors have been shown to reduce rosacea symptoms.
Related article: NLRP3, genes and elevated inflammation
Recap: All of this comes together in the ways that inflammatory pathways interact. Activation of toll-like receptors leads to cathelicidin production. Cathelicidin activates the MRGPRX2 receptor on mast cells. Mast cells release histamine and inflammatory cytokines causing vasodilation and triggering an inflammatory cascade. TRPV channels alongside mast cells are activated, triggering pain and blood vessel formation, and TRPV channels on mast cells can be activated by heat, triggering mast cell degranulation.
Blood flow, vasodilation:
In addition to inflammation, rosacea is known for redness and small capillaries that appear on the surface of the skin. Part of the inflammatory process is increased blood flow and growth of small blood vessels near the surface of the facial skin.
Inflammatory factors, including cathelicidins and TNF-alpha, lead to increased vascularization. Histamine released from mast cells also increases vasodilation.[ref]
The increased blood vessels near the surface of the skin cause the redness, flushing, and visible blood vessels in rosacea.
Skin barrier:
A recent study showed that people with rosacea have a more permeable skin barrier than normal. The study looked at the tight junctions and the depth of permeability in rosacea skin and found that there was increased permeability at 8μm on the face.[ref] Another study explains that in rosacea, certain pathways related to the skin barrier are altered so that the permeability is increased. In people with papulopustular rosacea, the skin barrier alterations were found near sebaceous (oil) glands and hair follicles. [ref]
Triggers and environmental factors:
What triggers immune system activation? This is where environmental factors come into play.
The skin microbiome is altered in rosacea, and microscopic skin mites are often increased. This is combined with environmental triggers that worsen or flare rosacea, including UV radiation (sunburn), wind, extreme heat or cold, and air pollution. Diet, stress, and alcohol, all of which affect overall systemic inflammation, can make rosacea worse. Exposure to certain skin care products may also come into play – all of which comes back to the interaction with skin microbes and the inflammatory response.
Skin microbiome in rosacea:
It makes sense that the skin microbiome can play a role in the inflammation seen in rosacea. We all have bacteria on our skin, and there is a balance between healthy skin, microbes, and immune response.
A study in twin pairs, where one had rosacea and the other didn’t, clearly shows the role of bacteria in activating the inflammatory response. The study showed that there were changes in the levels of certain genera of bacteria that are found in low abundance on normal skin. There was an increase in Gordonia species and a decrease in Geobacillus species in rosacea.[ref]
Other studies have also found that the skin microbiome is altered in people with rosacea. The studies found that certain bacterial species are depleted, while other normal skin bacteria are overabundant.[ref]
Demodex mites:
In addition to microbes on the skin, most people also have microscopic mites on their skin and hair follicles. While this is usually tolerated at some level, researchers believe that Demodex mite infestations cause inflammation in papulopustular rosacea.[ref]
A study of 242 patients with face papulopustules showed that the density of Demodex mites was associated with facial redness and papulopustules.[ref] Other studies point to a combination of Demodex mites along with certain bacteria that live on the mites.[ref]
Skin mites and bacteria on the skin are normal (whether we like to think about it or not). However, the difference in rosacea is that the immune response to the mites and certain bacteria is different from normal. There’s an over-activation of inflammation, which then causes the cascade of events that leads to redness, irritation, skin permeability, and increased capillaries.
Environmental triggers:
Exposure to UV rays can make rosacea worse for some people. UV radiation can increase oxidative stress in cells. Cold or heat is another common environmental trigger.
Cosmetics and skin care products can often irritate and worsen rosacea symptoms. One study showed that rosacea patients with a more permeable skin barrier had increased skin irritation to common skin care ingredients such as sodium lauryl sulfate.[ref]
Here’s a schematic drawing from a review article summing up the causes and pathways involved in rosacea:[ref]
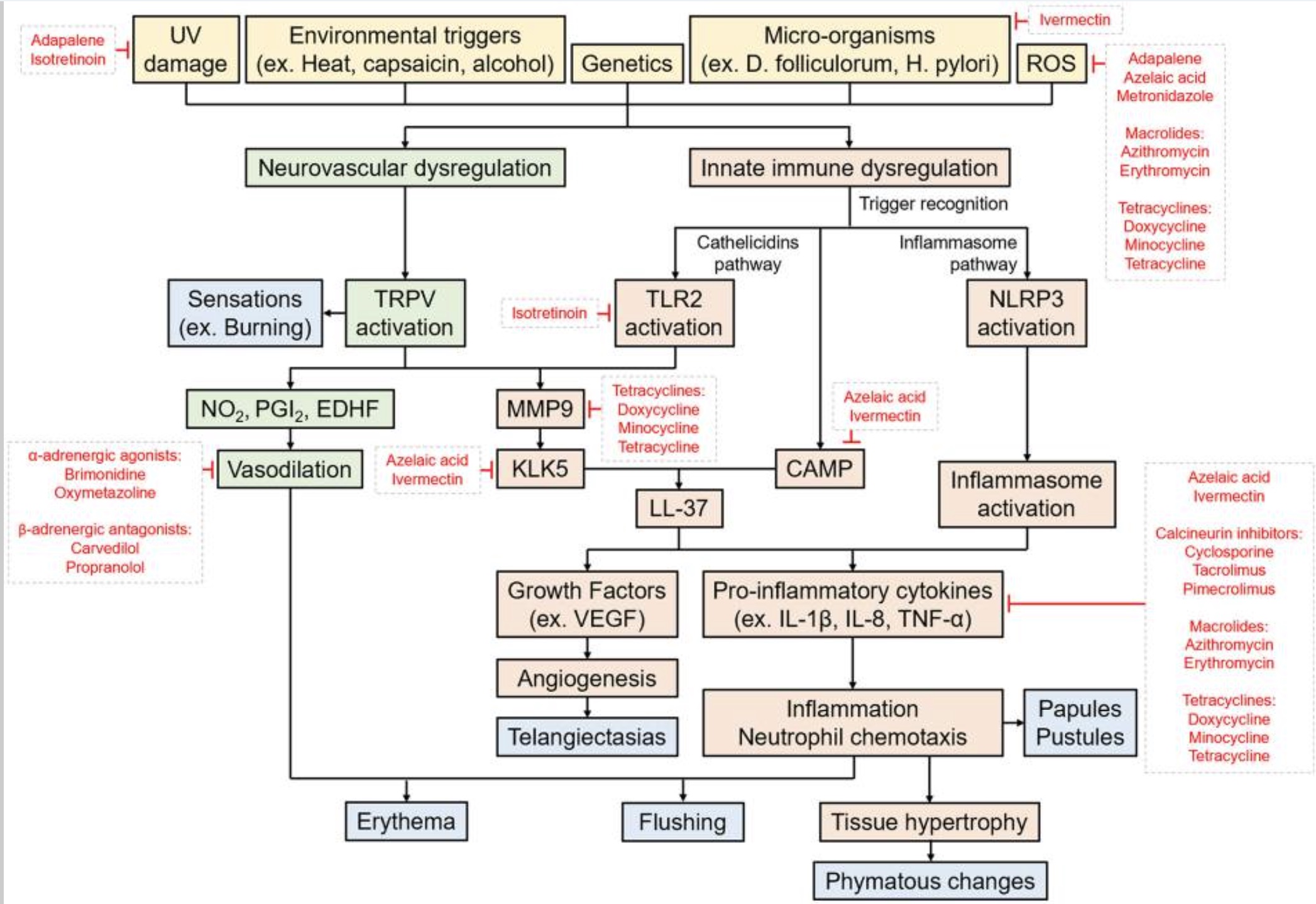
Overall inflammation:
Increased inflammatory cytokines throughout the body may worsen rosacea.
- People with autoimmune diseases, alcohol abuse disorder, obesity, and diabetes are at an increased relative risk of rosacea.[ref]
- Smoking or being a former smoker increases the risk of rosacea by 2-fold.[ref]
- People with inflammatory bowel disease are at a higher risk of rosacea.[ref]
The flip side is also true. Reducing systemic inflammation reduces rosacea symptoms and risk. For example, eating a healthy diet rich in antioxidants reduces the risk of rosacea by more than 40%. [ref]
Genetic studies on rosacea:
Twin studies show that genetics play a role in who gets rosacea. One study showed about a 46% genetic contribution to rosacea.[ref]
Genes interact with environmental factors to trigger rosacea symptoms. For example, Demodex mites are commonly found on the skin and usually don’t cause an immune system response. However, higher levels of the mites upregulate TLR2 and trigger an immune response in some people who tend to have higher levels of inflammatory cytokines.[ref]
A 23andMe study found that several genetic variants related to increased inflammatory response were linked to rosacea risk. Additionally, melanocortin receptor (MC1R) variants were also increased the relative risk of rosacea. The MC1R gene encodes a receptor found in skin cells that produce melanin.[ref]
Vitamin D:
There are two types of vitamin D in the body – 25-hydroxyvitamin D3 [25(OH)D3 ] which is the inactive form and 1,25(OH)2D3 or calcitriol which is the active form. Vitamin D acts by binding to the vitamin D receptor (VDR) and activating the transcription of other genes. In the immune system, vitamin D can both increase the immune response, e.g. to a bacteria or pathogen, and it can modulate the immune response, such as in autoimmune diseases.
Serum 25(OH)D3 levels show the inactive form of vitamin D, which can be from supplements or from sun exposure. A study of 60 rosacea patients and 60 age and sex-matched healthy controls showed that high serum 25(OH)D3 levels were associated with a 36% increased risk of rosacea.[ref] However, another study found that having vitamin D above 25ng/dl decreased the risk of rosacea.[ref] Both studies showed that vitamin D receptor variants influence the risk of rosacea.
Genotype report:
This section covers the more common genetic variants that increase susceptibility to rosacea. There are also a handful of rare mutations that are linked to rosacea, but these aren’t included in 23andMe or AncestryDNA data.[ref] I’ve divided this into genetic variants related to inflammation and then genetic variants related to vasculature and skin formation.
Member Content:
Why join Genetic Lifehacks?
~ Membership supports Genetic Lifehack’s goal of explaining the latest health and genetics research.
~ It gives you access to the full article, including the Genotype and Lifehacks sections.
~ You’ll see your genetic data in the articles and reports.
Join Here
Lifehacks:
A dermatologist should be able to help you with your rosacea, and this is the first place most people start when looking for treatment options. The only FDA-approved oral treatment is a low dose of doxycycline, an antibiotic, but there are many other prescription topical treatments that a dermatologist can help you with. Topical options include antibiotics, antihistamines, and mite killers. For example, ivermectin is used for rosacea because it kills skin mites and reduces TNF-alpha. Some doctors prescribe beta-blockers to reduce the redness.[ref][ref]
However, with multiple underlying causes of inflammation, many times rosacea patients will end up trying multiple topical options before they figure out what works.
Again, this schematic of the pathways involved in rosacea is a good overview. The prescription medications are listed in red and show the pathways that they impact. Click on it for a larger view.
In addition to medications, laser therapy is also an option for rosacea. It may work especially well for rhinophyma (thick skin, red nose).[ref] Photobiomodulation may also be an option.
There are also natural options for rosacea that are often overlooked! Let’s take a look at the other options and the research that supports them.
Lifestyle and Diet:
Clean, antioxidant-rich diet:
A new study (March 2024) showed that a diet high in antioxidant-rich foods reduced the risk of rosacea by 40-45%, which is a pretty big impact. Participants in the study recorded their diets, and it was found that those who ate more antioxidant-rich foods were much less likely to have rosacea at all, and those who did have rosacea had fewer symptoms.[ref]
Avoiding spicy foods:
The TRPV channels are activated by spicy foods that contain capsaicin or cinnamaldehyde. Spicy foods can cause anyone to flush, and the flushing tends to be worse in people with rosacea. Dermatologists often recommend avoiding spicy foods to reduce flushing.[ref]
Alcohol consumption:
Drinking alcohol at any level is associated with an increased risk of rosacea.[ref] Alcohol at higher levels or in people with ALDH gene variants can cause flushing. Alcohol also affects your ability to metabolize histamine. Check your alcohol metabolism genes here.
Face masks:
Wearing face masks increases moisture and bacteria, leading to skin irritation. A number of studies show that wearing masks increases and worsens rosacea symptoms. In addition, the polypropylene material, fabric dyes, formaldehyde, and plasticizers in masks cause skin irritation.[ref]
Supplements and topical options for rosacea:
These are not in any particular order. I suggest looking at your genetic variants related to rosacea to see which pathways to target and then reading the references. Talk to your dermatologist if you have any questions.
Reducing mast cell degranulation:
Supplements that reduce mast cell degranulation, such as quercetin or luteolin, may help with rosacea.[ref] Before going overboard with luteolin or quercetin, you may want to check your COMT SNPs. People with slow COMT may find that high doses of luteolin and quercetin make them irritable or anxious.
Blocking MRGPRX2:
Osthole, a coumarin derivative found in Cnidium monnieri, has been shown in animal studies to block MRGPRX2 and reverse rosacea.[ref] Cnidium monnieri has been traditionally used in Chinese medicine for skin disorders. While Cnidium monnieri supplements are available online, most are in powdered form. I don’t know of any topical formulations that contain osthole.
Curcumin has also been shown to block the MRGPRX2 receptor activation in animal and cell studies.[ref]
Melatonin:
A targeted pathway analysis study showed that melatonin should help with rosacea by reducing inflammatory and vascular pathways. The study then tested the hypothesis using melatonin in mice with rosacea and on human rosacea skin tissue. The results showed that melatonin significantly reduced inflammatory cytokines and prevented the formation of aberrant blood vessels. [ref] Melatonin supplements are readily available (read my full article on melatonin), but I also wanted to point out that creams containing melatonin are also available.
Vitamin A:
Prescription retinols are often prescribed for rosacea, in part because they decrease the activation of TLR2[ref]. I’m not finding a lot of studies, though, on increasing vitamin A in the diet or through retinyl palmitate supplements. However, I would suggest reading about vitamin A, the conversion of beta-carotene, and your genes.
Targeting TNF-alpha:
If you have the TNF-alpha variant listed in the genotype report, targeting TNF may help reduce overall inflammation.
- Hesperidin:
A natural flavonoid found in citrus fruits, hesperidin (hesperitin) inhibits the release of TNF-alpha.[ref][ref] In a study of rosacea skin tissue, hesperidin decreased inflammation and redness.[ref] (Read more about hesperidin.) - Rosmarinic acid:
Found in rosemary, basil, holy basil, lemon balm, and perilla oil, rosmarinic acid is a natural TNF-alpha inhibitor.[ref] One study found that topical rosmarinic acid along with caffeic acid reduced redness in rosacea patients.[ref]
Artemisinin:
A traditional Chinese herbal therapy, artemisinin has been shown in animal studies to reduce inflammation in rosacea. In addition, artemisinin blocked the growth of new blood vessels in the face.[ref]
Tea Tree Oil:
.
Tea Tree Oil:
Tea tree oil is often used to kill Demodex mites. Tea tree oil is extracted from the Melaleuca tree, and several components of the oil kill Demodex.[ref] A clinical trial using tea tree oil along with permethrin (insecticide) showed significant improvements in rosacea after 12 weeks.[ref] Of note – pure tea tree oil can be harsh on the skin. For eyelid mite infestations, tea tree oil is used at concentrations of 5-50%, but stinging and irritation are common side effects. Consult your dermatologist for recommendations on this.
Ivermectin:
Topical ivermectin cream has been shown in multiple studies to kill Demodex mites and also tamp down inflammation in rosacea.[ref][ref][ref] You can get ivermectin cream over the counter or by prescription.
Hyaluronic acid:
A small study showed that low-molecular-weight hyaluronic acid helped to normalize the inflammatory response in the skin.[ref][ref]
Just a note: Low molecular weight hyaluronic acid is available as a powder, and there are a number of websites that explain different ways to make your own serum without fragrances and additives (e.g. just hyaluronic acid plus distilled water…). I’m mentioning this for anyone who has skin that’s sensitive to all the extra ingredients often found in commercial hyaluronic acid serums.
Niacinamide:
A vitamin B3 derivative, nicacinamide or nicotinamide may help with skin barrier function. It is often recommended topically for rosacea.[ref][ref] A clinical trial of an oral supplement that included nicotinamide, zinc, and folate improved skin in 79% of rosacea patients.[ref]
Zinc:
Zinc is essential for modulating the immune response. One placebo-controlled trial found that 100mg/day of zinc sulfate reduced symptoms somewhat after three months.[ref] However, another clinical trial found that 220 mg of zinc sulfate per day didn’t improve symptoms.[ref]
It may be that people who are deficient in zinc have a better response to oral zinc supplements. Take a look at how much zinc you get in your diet using a tool like cronometer.com. Check your zinc genes here.
Aspirin:
An old-fashioned remedy, aspirin has been shown in studies to reduce inflammation and LL-37-induced rosacea in mice. Aspirin also blocked the increase in VEGF expression and stopped the inflammatory signaling. “Collectively we showed that aspirin exerts a curative effect on rosacea by attenuating skin inflammation and angiogenesis, suggesting a promising therapeutic candidate for the treatment of rosacea.”[ref]
Targeting NLRP3 inflammasome:
Check your NLRP3 genetic variants to see if you are more likely to have increased NLRP3 inflammasome activation (full article here):
| Gene | RS ID | Effect Allele | Your Genotype | Notes About Effect Allele |
|---|---|---|---|---|
| CIAS1 | rs35829419 | A | — | Increased NLRP3 activation |
| CIAS1 | rs1539019 | A | — | AA only: Increased NLRP3 |
| CIAS1 | rs10754558 | C | — | Somewhat increased NLRP3 activation |
| CIAS1 | rs3806265 | C | — | Somewhat increased NLRP3 activation |
| CIAS1 | rs10733113 | A | — | Somewhat increased NLRP3 activation |
| CIAS1 | rs12048215 | G | — | Somewhat increased NLRP3 activation |
| CIAS1 | i5007539 | G | — | Carrier of a mutation linked to familial cold urticaria |
| CIAS1 | rs28937896 | C | — | Carrier of a mutation linked to familial cold urticaria |
| CIAS1 | rs121908147 | A | — | Carrier of a mutation linked to familial cold urticaria |
| CIAS1 | rs121908150 | T | — | Carrier of a mutation linked to familial cold urticaria |
| CIAS1 | rs121908148 | G | — | Carrier of a mutation linked to familial cold urticaria |
If you have variants linked to increased NLRP3 activation:
- CBD oil decreases inflammation, in part, through inhibition of the NLRP3 inflammasome.[ref] There are also several studies on CBD oil for skin health including in acne and rosacea.[ref]
- Glycyrrhizin (in licorice) inhibits NLRP3 in cell studies and animal studies.[ref] Topical glycyrrhizin extract and injections of it may decrease redness and flushing in rosacea.[ref][ref][ref]
- EGCG, found in green tea, may help to suppress the activation of NLRP3. Research on EGCG in animal models of gout shows it to be effective in suppressing the activation of NLRP3 by urate crystal in gout.[ref] Studies also show that topical EGCG can decrease VEGF, but the very small clinical trial using a cream with 2.5% EGCG didn’t show much of a reduction in redness in rosacea patients after six weeks.[ref]
Recap of your genes:
| Gene | RS ID | Effect Allele | Your Genotype | Notes About Effect Allele |
|---|---|---|---|---|
| TNF | rs1800629 | A | — | higher TNF alpha, increased risk of rosacea |
| IRF4 | rs12203592 | T | — | increased risk of rosacea |
| IL13 | rs847 | T | — | increased risk of rosacea |
| HLA-DRA | rs763035 | A | — | increased risk of rosacea |
| NOD2 | rs2066844 | T | — | increased intestinal permeability, IBD; increased risk of rosacea |
| VDR | rs731236 | A | — | lower vitamin D levels; increased relative risk of rosacea with low serum vitamin D levels |
| VEGF | rs2010963 | G | — | increased risk of rosacea |
| MCR1 | rs1805007 | T | — | more photoaging, facial aging, increased relative risk of rosacea |
| HERC2 | rs1129038 | T | — | increased relative risk of rosacea |
[/mepr-show]
Related Articles and Topics:
MRGPRX2: Mast Cells, Itching, & Drug Hypersensitivity Reactions, Including Fluoroquinolones
About the Author:
Debbie Moon is the founder of Genetic Lifehacks. Fascinated by the connections between genes, diet, and health, her goal is to help you understand how to apply genetics to your diet and lifestyle decisions. Debbie has a BS in engineering from Colorado School of Mines and an MSc in biological sciences from Clemson University. Debbie combines an engineering mindset with a biological systems approach to help you understand how genetic differences impact your optimal health.


Hello i think that i saw you visited my weblog so i came to Return the favore Im trying to find things to improve my web siteI suppose its ok to use some of your ideas
Hi Neat post Theres an issue together with your web site in internet explorer may test this IE still is the marketplace chief and a good component of people will pass over your fantastic writing due to this problem